Keep Your Policyholders Healthy — Before They File a Claim
AI-powered health record management that keeps insured patients engaged, informed, and proactive — reducing claim risk and improving policyholder retention.
AI-powered health record management that keeps insured patients engaged, informed, and proactive — reducing claim risk and improving policyholder retention.

Insurers spend heavily on acquisition, then lose policyholders to silence.
Insurers invest heavily in acquisition but lose engagement immediately after the policy is sold. Renewal conversations happen too late.
Without health monitoring, chronic conditions escalate silently. Early AI-powered detection reduces claim severity significantly.
Most policyholders do not understand their own coverage until they urgently need it, creating disputes and poor experiences at critical moments.
Five capabilities that turn passive policyholders into engaged, proactive health participants.
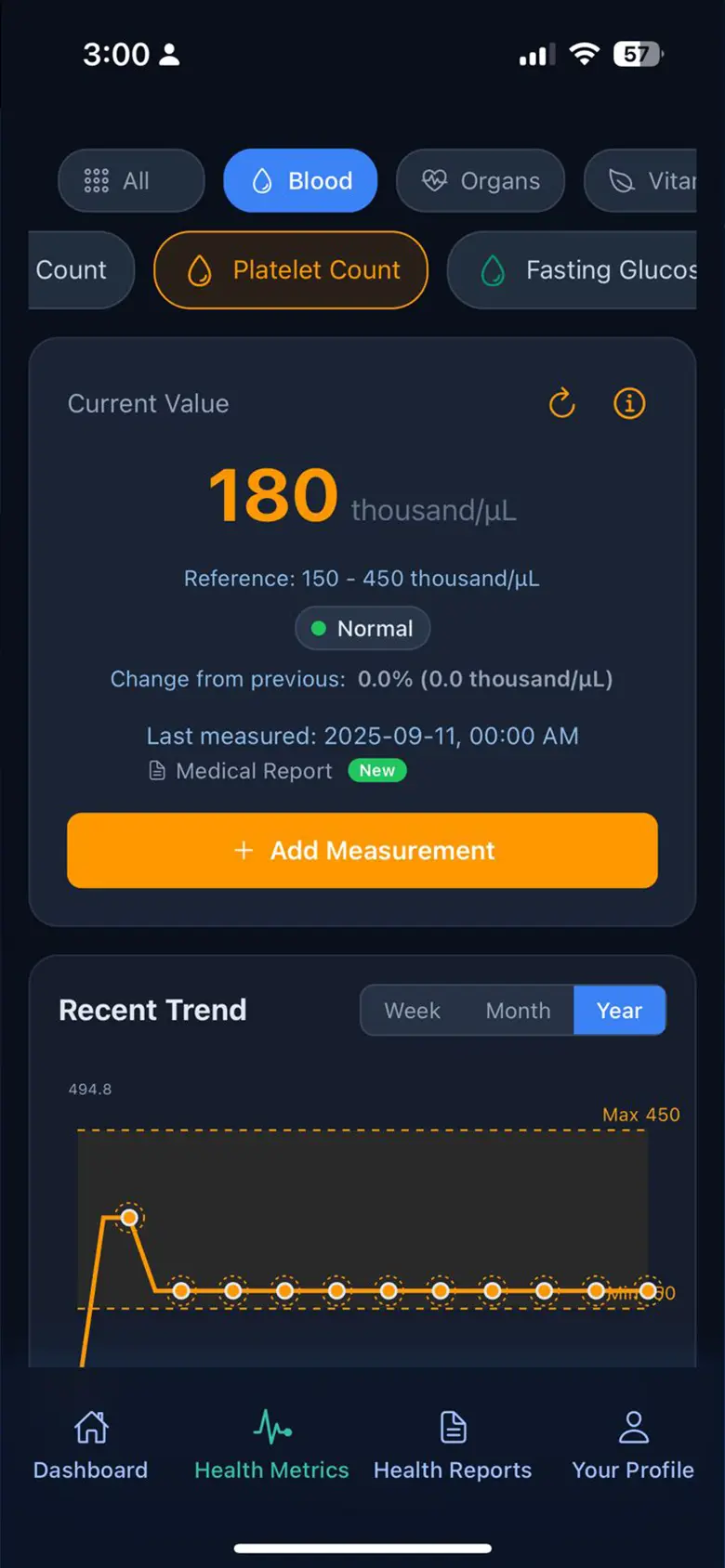
Policyholders upload lab reports and receive instant AI summaries. 70+ health parameters tracked automatically with trend alerts for abnormal values.
Policyholders upload their insurance document and ask plain-language questions: What is my coverage limit? What is excluded? How do I file a claim?
AI-driven reminders nudge policyholders to complete recommended tests based on their health profile, driving engagement between renewals.
One account for the entire insured family. Dependents tracked independently with separate health profiles — one view for all covered members.
All health updates, summaries, and alerts delivered on WhatsApp. No app download needed — reach policyholders on the channel they already use daily.
AI flags abnormal health parameters the moment a report is uploaded — enabling early intervention before conditions escalate into high-cost claims.
Flexible tiers designed to match your policyholder base and engagement goals.
Zero cost. Zero integration. Start in days.
What Your Company Gets
Deeper policyholder engagement at scale.
What Your Company Gets
Your brand. Your experience. Full strategic partnership.
What Your Company Gets
The data behind the value, and the platform principles that make it real.
Early AI detection of deteriorating health parameters enables timely intervention — reducing the likelihood of high-cost claims.
Health reminders, report summaries, and trend alerts keep your brand present between policy issuance and renewal — reducing churn.
Policyholders can ask plain-language questions about their own policy document — reducing disputes and improving claim satisfaction scores.
Family health management ensures every insured dependent has a health profile — maximising platform stickiness and household retention.
From policy onboarding to proactive health engagement — four simple steps.
Insurance company onboards policyholders onto the Webshark Health platform — via link, QR code, or co-branded invite.
Policyholders upload lab reports and insurance documents via the app or directly on WhatsApp — no technical friction.
AI generates health summaries, flags concerns, and delivers personalised insights to the policyholder's WhatsApp — instantly.
Insurer gains year-round engagement data. Policyholders stay proactive and connected between renewals — reducing lapse risk.
Tell us about your policyholder base and we'll walk you through your best partnership option.